Managing vaccinations

Vaccines are medicines which are designed to stimulate the immune system.
Animals can be vaccinated against viruses, bacteria or parasites so that when they encounter these pathogens for real they are more able to fight off the infection.
Vaccines can be live or inactivated.
Advertisement
Advertisement
Live vaccines generally contain the whole virus or bacteria which has been altered in some way so that it will not cause disease, but because it is live it can still multiply in the animal, exposing the animal to a more ‘realistic challenge’. Live vaccines usually come in two parts; a freeze dried pellet and liquid. Once mixed the vaccine should be administered as soon as possible. Rispoval® IntraNasal is an example of a live vaccine and is commonly used for prevention of respiratory disease in young calves from nine days of age.
Inactivated vaccines contain a killed pathogen or part of a pathogen (an antigen). Adjuvants are then added to the vaccine to enhance the immune response. The adjuvant helps overcome the fact the antigen won’t multiply in the animal. Inactivated vaccines typically come in a ready to use formulation. They should still be used as soon as broaching the vial (typically eight to 10 hours) because of the risk of introducing contamination. Rispoval® IBR Marker Inactivated is an example of an inactivated vaccine commonly used to control IBR in adult beef and dairy herds.
How do they work?
Vaccines expose the animal’s immune system to the virus, parasite or bacteria in a safe way.
This has two functions:
1) Enhanced resistance to disease:
The immune system is primed. If later challenged the animal’s immune system responds more quickly and therefore the vaccine reduces the risk of disease.
2) Reducing viral and bacterial exposure:
Advertisement
Advertisement
Sick or infected animals can shed large quantities of viruses and bacteria, which can infect neighbouring animals. Vaccination reduces both the number of sick animals and the amount of virus or bacteria shed by sick animals so reducing risk to neighbouring animals.
Therefore in a non-vaccinated herd, in the face of a disease challenge, animals are more at risk of becoming infected. Animals in vaccinated herds are more resistant to disease and therefore fewer animals are likely to be affected, and less virus and bacteria are shed in the environment. In a vaccinated group, fewer animals are susceptible to new infection and the population as a whole is more resistant to disease
Setting realistic expectations:
In an ideal world we would want our vaccines to achieve 100% protection, 100% prevention of clinical signs, prevention of spread of infection and perhaps even eradication.
Realistically vaccination in most cases is more likely to achieve a reduction of clinical signs, reduction of shedding and overall a reduction of infection at the flock/ herd level.
Advertisement
Advertisement
This is of course very vaccine specific. For example we expect total protection when using clostridial vaccines, whereas cattle respiratory vaccines will reduce, but not completely prevent disease. Hence why vaccination is often part of a wider solution, which can also involve management changes.
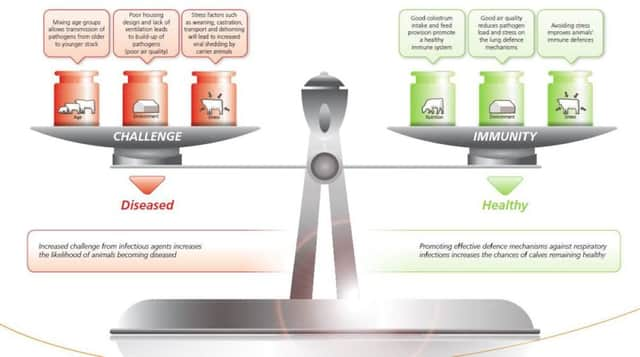
Disease control is a balancing act. It is all about maintaining the balance between challenge and immunity. Increased challenge from infectious agents increases the likelihood of animals becoming diseased.
Using respiratory disease as an example, factors which can increase challenge include:
-Mixing age groups as this will allow transmission of pathogens from older to younger stock.
Advertisement
Advertisement
-Poor housing design and lack of ventilation which will lead to build-up of pathogens as a result of poor air quality.
-Stress factors such as weaning, castration, transport and dehorning will lead to increased viral shedding by carrier animals.
Promoting effective defence mechanisms against respiratory infections increases the chances of animals remaining healthy.
Examples of increasing the animals’ immunity are:
-Good colostrum intake and feed provision to promote a healthy immune system.
Advertisement
Advertisement
-Good air quality reduces pathogen load and stress on the lung defence mechanisms.
-Avoiding stress improves the animal’s immune defences.
Vaccination can help you tip the balance between challenge and immunity in your favour.
Five considerations for Vaccine Selection:
1. Cover against the likely pathogens for the full risk period
Choose a vaccine that protects against the viruses/bacteria present on your farm for a sufficient period of time (e.g. 6m, one year or the winter housing period).
2. Ensure protection is in place BEFORE challenge
Advertisement
Advertisement
The vaccination course needs to be completed before the challenge
Vaccines do not work immediately - ‘onset of protection’ can vary from a few days to two to three weeks. Some vaccines for example will require two injections and full onset of immunity won’t occur until about two weeks after the second injection.
If vaccine can’t be given early enough then you may need to consider single dose intranasal vaccines for faster onset?
3. Consider the animal’s environment and need to vaccinate ALL animals within an airspace or pen
Advertisement
Advertisement
Vaccination in many instances is a HERD/GROUP strategy (remember that the role of vaccination is two fold; increase immunity, and reduce pathogen shedding)
Best results are often gained from vaccinating the whole group within an airspace or management group.
If an active decision has been taken not to vaccinate a particular group of calves, ideally these animals should be managed separately. In the case of BRD this means a separate airspace.
4. Age effect: passive immunity (from colostrum) can interfere with vaccination in young animals
Advertisement
Advertisement
Ensuring calves receive adequate colostrum is a vital part of overall management, but colostral antibodies can prevent some vaccines from working. The intranasal route helps overcome interference from maternally derived antibodies.
5. Avoid Stress:
Where possible avoid vaccinating at the same time as stressful procedures such as dehorning, castrating and weaning. The animal needs to ‘respond to’ the vaccine and stress can reduce its ability to do this, preventing the vaccine from working effectively.
Vaccine Storage
Most vaccines need to be stored in a fridge storage at a temperature range of +2 to +8oC. Live vaccine are very sensitive to elevated temperatures whereas inactivated vaccines are more sensitive to freezing.
A study run from January to August 2014 involving 19 farms monitored the temperature inside the fridges every 30 minutes. ALL the fridges were outside the required temperature range on at least one occasion!
Advertisement
Advertisement
The minimum fridge temp recorded was -12oC. The fridge temperatures tended to exceed 8oC from May through to August. The external temperature was clearly affecting the ability of the fridges to maintain a low temperature. Some fridges were quite simply acting as cupboards in disguise! If you are investing in vaccines you want them to work, so make sure that your fridge is in good working order.